Cite This Work
- APA
- MLA
- BibTex
@inproceedings{simonian2026beyond,
title={Beyond the Testing Room: Virtual Reality as a Paradigmatic Solution to Ecological Validity Deficits in Neuropsychological Memory Assessment},
author={Simonian, Ninette and Reggente, Nicco},
booktitle={Virtual Worlds},
volume={5},
number={1},
pages={7},
year={2026},
organization={MDPI}
} Beyond the Testing Room
If you’ve ever sat across from a clinician and been asked to memorize a list of unrelated words like “apple, car, justice, umbrella” and then repeat them back, you’ve experienced the standard of neuropsychological memory testing. These tests have been used for decades. And according to a new perspective paper from our lab at the Institute for Advanced Consciousness Studies, they may be falling short for the very people who need them most.
The Problem With Word Lists
Imagine you’re worried about your memory. You’ve been misplacing your keys, forgetting names mid-sentence, losing track of why you walked into a room. You go to a neurologist. They sit you down and ask you to memorize words, copy geometric shapes, and count backwards from 100. You score fine. The doctor reassures you.
But the things you’re actually struggling with, like cooking a meal without losing track of steps, remembering to take your medication, or navigating a familiar neighborhood, none of those were tested. According to our new research review, that gap isn’t a minor inconvenience. It could mean that early signs of cognitive decline are being missed.
One of the latest papers from IACS, published in the journal Virtual Worlds, argues that traditional memory assessments have a fundamental limitation: they measure memory in environments so stripped-down and controlled that they tell us relatively little about how memory actually works in daily life. We call this an “ecological validity” problem. The tests don’t reflect the real world closely enough to meaningfully predict how someone will function in it.
The Four Shortcomings of Traditional Tests
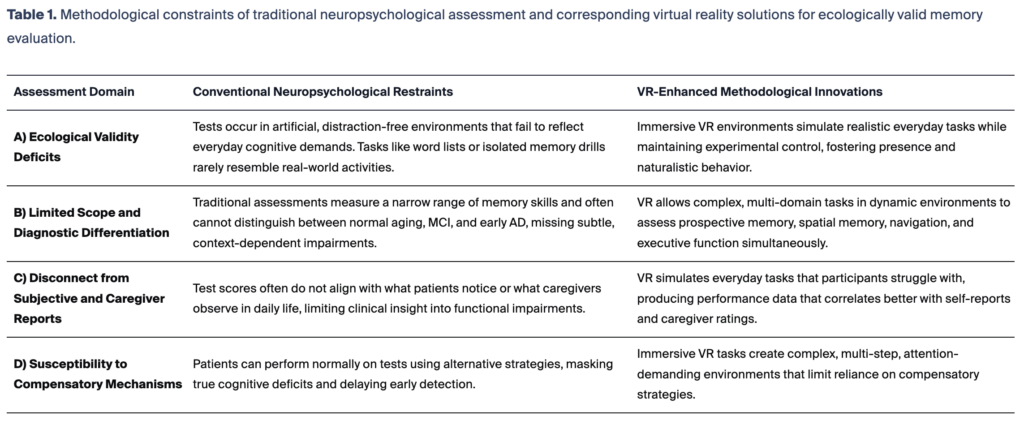
We identified four specific ways traditional tests fall short.
First, they lack real-world relevance. Memorizing unrelated words is a task almost nobody encounters in daily life. Real memory challenges, like remembering a prescription, navigating to a new doctor’s office, or tracking a multi-step recipe, are nowhere to be found in the testing room.
Second, traditional tests struggle to distinguish between stages of decline. Telling apart healthy aging from mild cognitive impairment (MCI), or MCI from early Alzheimer’s disease, requires detecting subtle differences. Standard tests often can’t catch these gradations until the disease has already progressed significantly.
Third, test scores frequently don’t match what patients and caregivers report. Someone might score normally on a word-list test while their spouse notices them getting lost on familiar routes or forgetting appointments. The disconnect isn’t because one party is wrong. It’s because the test is measuring something different from what matters in everyday life.
Fourth, people can perform well on these tests even as their brains are genuinely changing. Because the tasks are simple and predictable, the brain can compensate by recruiting alternative neural circuits to maintain performance. By the time that compensation fails, the opportunity for early treatment may have already passed.
Enter Virtual Reality
The solution we propose is virtual reality (VR), a technology that places users inside a fully computer-generated, three-dimensional environment, typically experienced through a headset. Unlike augmented reality, which overlays digital elements onto the physical world, VR replaces your surroundings entirely. What makes VR particularly well-suited for clinical assessment is that it combines two things that are hard to achieve simultaneously: immersion in realistic, lifelike scenarios and precise experimental control. A clinician can administer a virtual grocery store task that looks and feels like real life while ensuring every patient encounters the exact same environment, distractors, and timing. That level of standardization is difficult to achieve with real-world observation and impossible with paper tests.
VR-based assessments place patients inside realistic, interactive environments including virtual grocery stores, kitchen simulations, and neighborhood walks that mirror the actual cognitive demands of daily life. Instead of memorizing the word “apple,” a participant navigates a store aisle to find apples, manages a virtual budget, and filters out distracting announcements over the PA system. These tasks engage memory the way life does: as part of a complex, multitasking, spatially-grounded experience.
The diagnostic results have been encouraging. One VR spatial navigation test achieved 94% sensitivity and 96% specificity in distinguishing people with MCI from healthy older adults, outperforming standard cognitive screeners. Another VR task correctly classified 87% of MCI patients based on their behavior in a virtual supermarket. In one particularly notable study, a VR path-integration task (assessing the brain’s ability to keep track of where you are in space as you move through an environment) detected early Alzheimer’s-related brain changes in young adults who were genetically at risk, changes that showed no trace on standard memory tests.
Why Space Matters
A central idea in our paper is that memory and space are closely linked. The brain regions most vulnerable to early Alzheimer’s, particularly the entorhinal cortex (located in the medial temporal lobe) and hippocampus, are also responsible for spatial navigation and building mental maps of our environment. When these areas begin to change, one of the early consequences is difficulty orienting ourselves in space.
By requiring patients to navigate virtual environments, update their position as they move, and remember where things are located, VR engages the neural circuits that are most relevant for early detection.
We also focus on what’s called “feature binding,” the brain’s ability to connect what happened, where it happened, and when. This integration is what makes an experience feel like a complete memory rather than an isolated fact. Hippocampal changes disrupt this binding, and older adults show deficits here well before simpler memory skills decline. Because VR tasks require this kind of rich, contextual memory, they are better positioned to catch what traditional tests miss.
Better Alignment With What Patients and Families Experience
One of the more meaningful findings we reviewed is that VR performance tends to correlate more closely with patients’ own experiences and their caregivers’ observations than traditional test scores do. Someone who feels their memory is slipping may score normally on a word list, but their performance in a virtual environment often reflects the difficulties they’re actually living with.
This matters both clinically and practically. When a patient’s family notices real-world difficulties that the doctor’s tests don’t reflect, it can create friction around questions of driving, independence, and whether concerns are being taken seriously. VR assessments could help by providing data that more closely matches what families are observing at home.
Real Promise, Real Challenges
We want to be clear about the hurdles that remain. VR headsets can cause nausea and disorientation, particularly in older adults, and physical discomfort could affect performance and make results harder to interpret. Older adults who are less familiar with technology may also find the interface itself challenging, making it difficult to separate cognitive difficulties from unfamiliarity with the device.
There are also practical considerations in clinical settings. VR systems take time to set up, clinicians need training, and physical space may be required. There is also not yet enough standardization across VR platforms, which makes it difficult to compare results across clinics or establish reliable cutoff scores for diagnosis.
We call for more rigorous validation work, standardized protocols, and larger, more diverse studies. VR assessment is not ready to replace traditional testing, but it is ready to be taken seriously as a useful complement to it.
The Bigger Picture
Cognitive decline within the “silver tsunami” is one of the most pressing public health challenges today. Alzheimer’s disease is among the most feared diagnoses for American adults. Without a cure, early detection remains critical for accessing the most effective interventions to at least mitigate symptoms and decelerate progression. That requires tools that can capture what’s actually happening in the brain, not just what’s easiest to measure in a clinical setting.
VR offers something traditional assessment has not been able to: a way to observe memory functioning in conditions that more closely resemble real life. We believe VR represents not just a better test, but a meaningful shift in how we think about memory assessment, one that evaluates memory in the dynamic, spatial, and contextually rich environments where it naturally operates.